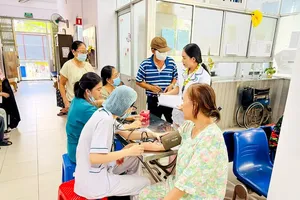
In Ho Chi Minh City, a segment of informal workers, primarily migrants, remains outside the health insurance system, has not registered for temporary residence, and has limited access to primary healthcare services. This situation poses challenges for health management amid constant population mobility. In response, commune- and ward-level health facilities have been identified as playing a crucial role in reaching, managing, and providing care for this group.
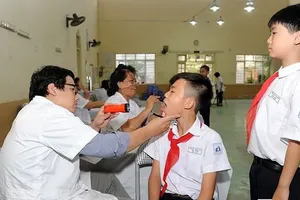
Under the harsh midday sun, a 37 year old delivery driver from Vinh Long, suddenly collapsed by the roadside after hours of continuous work. He was taken to a health station in Tan Thuan Ward for emergency care. Medical staff found that he had not enrolled in health insurance and had never undergone a routine health check-up. Living in a cramped rental room in Tan Thuan Ward without a temporary residence registration, his health records were virtually nonexistent. The delivery driver said he typically self-medicates for minor illnesses and only goes to the hospital when his condition becomes severe.
Among migrant and freelance workers, those without temporary residence registration or health insurance are not uncommon, creating significant difficulties for local authorities in compiling medical records and monitoring health conditions.
Beyond central Ho Chi Minh City, many areas bordering industrial zones have seen large concentrations of migrant workers in rental housing and residential clusters, driving up demand for healthcare services. Wards such as Phu My, Tan Uyen, Di An, Binh Duong, An Phu, Tan Khanh, Binh Chuan, Vinh Tan, Ben Cat, and Bau Bang Commune host large numbers of workers and informal laborers, placing increasing strain on grassroots healthcare systems.
HCMC has recently issued a plan for regular health check-ups and screenings for residents during the period of 2026-2030, aiming to gradually organize examinations at least once a year and update the information in electronic health records.
Notably, the city is expanding the target group to include those outside the formal labor system (such as informal workers, small traders, farmers, fishermen, and homemakers - individuals who have historically received little health management).
Health check-ups will be conducted at qualified medical facilities, and mobile services may be organized when necessary. The funding for these health examinations will come from the state budget, health insurance funds, and other legal sources.
In response, local health stations have maintained periodic health check-ups and management of non-communicable diseases, while facilitating migrants’ access to basic services such as initial examinations, vaccinations, health consultations, and disease prevention. However, pressure on primary healthcare remains substantial, especially following administrative mergers and sharp population fluctuations. The establishment of health records and epidemiological monitoring continues to face obstacles, while the risk of disease emergence and spread increases without close surveillance.
Burden of treatment in the absence of health insurance
One of the key bottlenecks in providing healthcare for informal workers is the low or inconsistent rate of health insurance participation. According to Dr. Mai Duc Huy, Deputy Director of Gia Dinh People’s Hospital in Ho Chi Minh City, the main reason is that this group does not enroll in health insurance through companies or employers, but must instead pay independently under household or voluntary schemes. Meanwhile, their incomes are unstable and awareness of the benefits of health insurance remains limited.
Vietnam’s health insurance coverage currently reaches about 95 percent of the population. The uninsured segment includes many informal workers and migrants. This group also faces higher health risks due to the nature of their work, which often involves heavy labor, long working hours, and frequent exposure to occupational and traffic accidents.
In this context, the grassroots healthcare system, particularly commune- and ward-level health stations, plays a critical role in primary health management for informal workers. With strengthened staffing, improved professional capacity, and better equipment, along with the addition of basic paraclinical services such as ultrasound and laboratory testing, these local health stations could become the closest point of care, enabling early disease detection and reducing pressure on big hospitals.
At the same time, various measures are being implemented to expand health insurance coverage. These include strengthening communication in communities, diversifying outreach through digital platforms, and making it easier for residents to register for health insurance via the VssID application and the National Public Service Portal. The goal is to raise coverage to around 95.5 percent of the population by 2026, thereby reinforcing the role of primary healthcare in community health management.