Escalating pressures
Healthcare is a distinct domain, inextricably intertwined with the individual lives of all citizens. Consequently, it’s common for everyone to voice an opinion. A professor from the National University of Singapore once posited that regarding health or education, any citizen might speak as if they’re a “Minister.” This observation captures the sector’s intimate yet complex nature.
Vietnam has recently delineated clear strategic paths for the healthcare sector. Resolution No. 20-NQ/TW, issued on October 25, 2017 by the 12th Party Central Committee, serves as the inaugural comprehensive healthcare mandate, establishing a vital framework for system innovation.
Subsequently, Resolution No. 72-NQ/TW, dated September 9, 2025, introduces further pioneering solutions, maintaining a steadfast focus on Primary Healthcare (PHC) as the fundamental cornerstone. This sound trajectory aligns with the global mission of fostering healthy lifestyles and enhancing well-being across all age groups.
However, a notable disparity reportedly remains between official policy and practical execution. Works to establish a health system with PHC as its sustainable, systemic pillar haven’t yet reached anticipated benchmarks. Financial resources aren’t the only bottleneck; the issue also stems from inconsistent approaches and a lack of synchronized implementation across various levels of governance.
It's evident that the healthcare system is confronting unprecedented challenges. Public demand for healthcare is rising, both in terms of the quantity and quality of services. Accompanying this is a rapid population aging process, leading to a surge in non-communicable chronic diseases.
While the health system previously focused primarily on acute and infectious diseases, the disease burden has now shifted markedly toward cardiovascular diseases, cancer, diabetes, chronic obstructive pulmonary disease, and mental disorders. These conditions require long-term, continuous management that relies heavily on primary care.
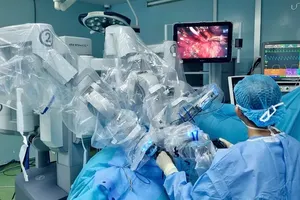
Furthermore, the Covid-19 pandemic served as a powerful warning about the vulnerability of the national health system to global shocks. Simultaneously, the rapid evolution of science-technology, AI, and precision medicine demands constant updates, innovation, and adaptation. All these factors create a combined pressure, forcing Vietnam to re-examine the organization and operation of the health system more fundamentally.
One of the most notable achievements in the health sector recently is the rapid increase in the number of medical doctors. From 5.3 doctors per 10,000 people in 2001, the nation reached 9.81 in 2020 and 12.5 in 2023, surpassing the targets of Resolution 20. If the training rate of approximately 12,000 doctors annually is maintained, Vietnam can certainly achieve, or even exceed, the goals of 15 doctors per 10,000 people by 2025 and 19 by 2030.
Regrettably, numbers aren’t everything. The primary challenge lies in training quality and the practical competence of graduates. Chasing quantity without ensuring quality could lead to a heavy long-term price regarding treatment efficacy and public trust.
Furthermore, human resource distribution remains uneven. Medical doctor ratios in the Central Highlands and Mekong Delta are significantly lower than in major urban centers, causing healthcare disparities. Nurses, the backbone of patient care, also remain in short supply, with ratios lagging behind regional peers. Meanwhile, a neglect of specialized personnel roles is wasting “golden population” resources.

“Inverted pyramid” paradox and systemic approach
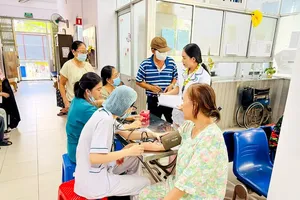
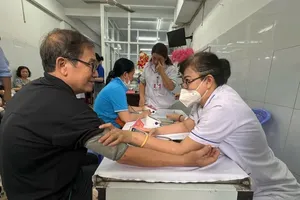
A striking paradox currently plagues the distribution of medical human resources. According to WHO estimates, primary healthcare can address 80-90 percent of an individual’s lifelong health needs, necessitating a heavy concentration of resources at the grassroots level.
In reality, however, resources gravitate toward higher-tier institutions, leaving local facilities financially and professionally starved. Consequently, Vietnam’s “inverted pyramid” forces patients to bypass local clinics, overwhelming top-tier hospitals while leaving lower levels dormant.
Flipping this pyramid requires addressing why professionals should choose and stay at the grassroots. Currently, training is tethered to specialized hospitals, orienting students toward large centers. Without decisive policy intervention, Adam Smith’s “invisible hand” simply can’t bridge this systemic supply-demand gap.
To address these mounting pressures, a more systemic approach is undeniably required. The Lancet Commission on Education of Health Professionals has emphasized that the healthcare system must effectively “place orders” with the training sector regarding the specific type, quantity, and quality of personnel needed.
This necessitates seamless coordination between health and education; at the end of the day, it’s impossible to let these two systems operate in silos. Simultaneously, it’s essential to vigorously innovate training methodologies, ranging from curriculum content to practical organization, ensuring graduates possess the requisite competence for real-world environments, particularly at the grassroots level.
Several reformative pathways warrant serious consideration. First, the medical training system should be restructured to align with regional demands. Disadvantaged areas reportedly require bespoke training and recruitment policies tailored to their unique circumstances. Furthermore, it’s compulsory to bolster the training of general practitioners, family doctors, and nurses, the frontline vanguard of primary care.
Developing novel personnel roles is another viable strategy to alleviate the physician’s burden. For instance, a Bachelor of Ultrasound could perform scans, freeing up doctors for more complex diagnostic tasks.
Moreover, a clear career trajectory for physician assistants is vital. Rather than a direct bridge to a medical degree, it’s wiser to establish distinct professional ranks like senior physician assistant, coupled with competitive remuneration to ensure they remain anchored at the local level.
Regarding local facilities, it’s essential to establish health station models equipped with appropriate technology and teams operating on family medicine principles. These units must be competent enough to fulfill the functions of ward or commune stations, including national programs and primary care.
Eventually, utilization and remuneration policies must be redesigned to incentivize personnel at lower levels. Mandatory service periods at the grassroots level post-graduation could also be considered, coupled with income incentives, training opportunities, and promotion pathways. Implementing this systemically is paramount, as relying on irregular movements or voluntary efforts simply lacks long-term sustainability.
Towards sustainable health system
Building a health system anchored in primary healthcare is entirely feasible, yet it demands a long-term vision and persistent implementation. Such a system extends beyond treatment tiers; it encompasses macro policies like finance, insurance, and public investment. These factors are inextricably linked, meaning piecemeal reforms won't achieve overall efficiency.
While national directions align with international trends, the challenge lies in practical execution. This journey requires unwavering policy consistency and synchronized coordination across all sectors. Ultimately, success depends on the collective participation of management, institutions, and every citizen, starting with that vital first step toward a sustainable future.