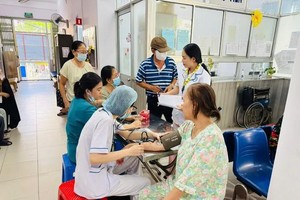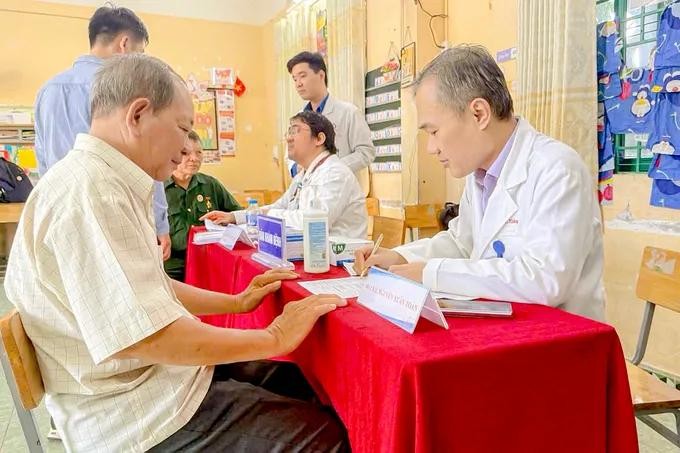
The rapidly aging population is placing increasing pressure on the social security system in the country. While life expectancy continues to rise, the number of healthy years has not kept pace, leading to a growing burden of chronic disease, higher healthcare costs, and rising demand for long-term care.
At the same time, gaps in geriatric services remain significant, falling short of actual needs and posing mounting challenges for families, the healthcare sector, and society at large.
For 86-year-old Le Thi Hong Thuy, the twilight years have become a source of profound distress, marked not by solitude but by the discord of her own children. Despite residing in her own home, the Dong Nai resident now finds herself at the center of a family fracture as her children clash over the logistics of her care.
Ms. Thuy, whose independence has sharply declined, now requires full-time assistance. However, her four children—all of whom are retirees with their own family obligations—have struggled to reach a consensus on caregiving schedules. As Ms. Thuy’s cognitive health continues to deteriorate, the resulting family friction has turned what should be a support system into a source of ongoing emotional hardship.
“In recent years, life has revolved around illness. I live closest to my mother, so the pressure is intense as we are both aging. My siblings, who live farther away, sometimes blame me for her condition, which is deeply hurtful. There are times I lose my temper with her, then lie awake all night in regret. Old age and illness are emotionally exhausting,” said Le Thi Nguyet, 62, Thuy’s daughter.
According to the Ministry of Health, Vietnam’s average life expectancy has risen significantly, from 65.5 years in 1993 to 74.7 years in 2025, surpassing many countries with similar income levels. However, much of this extended lifespan is spent in poor health, creating mounting challenges for the healthcare system as the proportion of older adults with chronic conditions continues to grow.
Nguyen Duc Cong, Vice Chairman of the Vietnam Association of Geriatrics, noted that Vietnam is among the fastest-aging countries in the world. The country currently has around 17 million elderly people, accounting for 16 percent of the population. This figure is projected to rise to 20.9 million by 2034, 27.5 million by 2044, and 38.5 million by 2074, placing sustained pressure on families, healthcare services, and social systems.
Pham Duc Muc, Chairman of the Vietnam Nurses Association, said older adults in Vietnam live with an average of 2.7 chronic conditions, with those over 80 typically facing four to five. As age increases, income often declines while dependency rises, leaving many elderly individuals reliant on family support and social welfare, particularly in accessing healthcare services.
Research shows that healthcare costs for older adults are two to three times higher than for younger populations. With limited financial capacity, many become increasingly dependent on health insurance and social assistance, while remaining vulnerable to prolonged medical expenses.
Gaps in specialized care
Despite rapid population aging and a growing elderly population, Vietnam’s system of elderly care services remains underdeveloped. Nationwide, there are just over 40 nursing homes and social protection centers offering professional care services—an insufficient number relative to the needs of approximately 17 million elderly people.
This shortage is placing considerable strain on both public healthcare systems and household finances. As hospitals become overcrowded and home-based care grows more burdensome, many families seek institutional care. However, the limited number of facilities, coupled with high service costs, means that a large proportion of elderly individuals continue to rely on family members or self-care.
Head Nguyen Van Tan of the Geriatrics Department at the Faculty of Medicine, University of Medicine and Pharmacy at Ho Chi Minh City, noted that Vietnam is “growing old before it becomes wealthy.” Many older adults live with chronic illnesses and declining health, while a comprehensive long-term care system has yet to take shape. Traditional multi-generational family structures are also changing, with smaller household sizes, increased migration, and economic pressures making home-based care more difficult.
He noted that many families face a dilemma that they want to care for their parents themselves but lack the time, knowledge, and resources to meet increasingly complex needs. Meanwhile, older adults face risks of loneliness, depression, and deteriorating health without proper care.
Data indicates that a basic elderly healthcare system has begun to form. Most provincial and municipal general hospitals now have geriatric departments, more than 900 outpatient units include dedicated services for older patients, and over 10,000 inpatient beds are prioritized for elderly care and rehabilitation.
Vietnam currently has three formal geriatric training programs at Hanoi Medical University, Hue University of Medicine and Pharmacy, and the University of Medicine and Pharmacy at Ho Chi Minh City. The National Geriatric Hospital serves as the leading institution, providing advanced treatment, rehabilitation, and professional training, while supporting lower-level facilities nationwide.
However, significant challenges remain, particularly in human resources. Geriatrics is still an emerging field in Vietnam, with limited investment. Formal training programs have only been established in recent years, and the number of doctors and nurses with specialized expertise in elderly care remains very small.
Experts note that even where geriatric departments exist at provincial hospitals, the quality of care can vary widely. In many localities, healthcare workers lack specialized training, increasing the risk of diagnostic and treatment errors.
Medical care for older adults requires careful adjustment. Standard prescriptions used for younger patients may pose serious risks if not calibrated to age-related changes in liver and kidney function. At the same time, shortages extend beyond physicians to include nurses and trained caregivers. In practice, most elderly care still relies on family experience or untrained domestic workers.
As a result, the three core pillars of geriatric care including disease prevention, rehabilitation, and mental health support, remain inadequately addressed. Many older adults therefore face not only physical illness but also loneliness and social isolation.





)